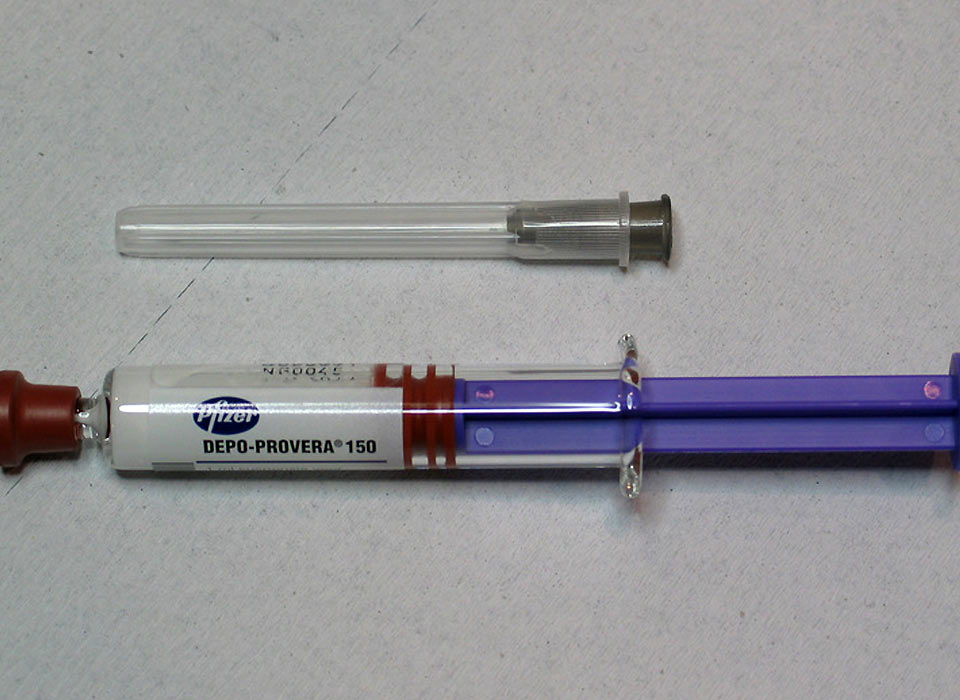
Common contraceptive could raise TB risk
15th April 2019
UCT Lung Institute World TB Day Events 2019
23rd April 2019Researchers from the University of Cape Town have found that the injectable contraceptive Depo-Provera could potentially increase women’s risk of contracting TB.
A breakthrough study by South African researchers, published in the Journal of Infectious Diseases in November last year, found that one of the country’s most commonly-used injectable contraceptives, Depo-Provera, could increase women’s chances of contracting tuberculosis (TB).
The study, led by Professor Keertan Dheda and Dr Michele Tomasicchio at the University of Cape Town’s (UCT) Centre for Lung Infection and Immunity, recruited women from Cape Town and looked at Depo-Provera and norethisterone enanthate (NET-EN) – two different injectable contraceptives commonly used in South Africa.
They found that Depo-Provera down-regulates immune function genes associated with protection against TB, and up-regulates certain cell types that suppress the immune system. The data also showed that, unlike Depo-Provera, norethisterone does not increase TB pathogenesis.
Injectable contraceptives are widely used across sub-Saharan Africa and are the birth control choice of over 16 million women in the region. According to the World Health Organization (WHO), some of the main reasons for their popularity include “their effectiveness, their simple re-injection schedule every two or three months, depending on the brand, and their sustainability for discreet use”.
Depo-Provera, HIV & TB
The growing concern of this contraceptive stems from a 2018 study of clinical data that found that Depo-Provera may increase women’s chances of contracting HIV by up to 40%. This is because the injection contains the synthetic hormone medroxyprogesterone acetate (MPA), which acts as an immunosuppressant.
The review revealed how MPA could affect the body’s immune system at a molecular and cellular level and increase the risk of acquiring HIV. In this study, NET-EN did, however, not increase women’s risk of contracting HIV.
Professor Dheda and Dr Tomasicchio considered the prevalence of TB in sub-Saharan Africa and the fact that it remains the top infectious disease killer globally, and realised the necessity of investigating whether Depo-Provera could also increase the risk of TB infection.
Policy change needed
Dr Tomasicchio would like to see the study results, along with those of future studies, drive a chance in policy surrounding the use of Depo-Provera in South Africa. “My ultimate aim is to make sure that women are aware of the dangers of using [Depo-Provera], particularly in the context of sub-Saharan Africa,” he said, adding that government clinics in South Africa – and elsewhere – should move over to NET as it is the safer choice.
On average, injectables are the contraceptive choice in 25% of cases in South Africa, but it is used in up to 85% of KwaZulu-Natal’s rural clinics.
However, despite the studies’ findings, the government is still reluctant to change policies since Depo-Provera is cheaper to manufacture and maintain. It also works on a three-monthly reinjection schedule, while NET-EN must be administered every two months.
Dr Tomasicchio says he plans to pursue this study further to gain a better understanding of why and how MPA actually drives TB pathogenesis. He also hopes that the mounting evidence of these studies will be taken to heart by the South African government and that policy changes will be made sooner rather than later.
Read more, Health24, 18 April 2019
Photo: www.freepik.com